The So-called “Near Collapse” at the Frontline of Japanese Medical and Nursing Care Services
As with other countries around the world, the spread of COVID-19 in Japan, directly struck healthcare facilities and care homes for the elderly. By early May 2020, a total of 250 cases of mass infections (cluster infections) had broken out across Japan. Of those, 85 cases occurred in medical institutions and 40 cases in senior care facilities (Mainichi Shimbun, 13 May, 2020). These brought about the deaths of many residents and hospital patients. According to a survey conducted by NHK, more than 550 people became infected at care homes around the country with 60 residents confirmed dead by the end of April (NHK NEWS WEB, 8 May, 2020).
At some of these facilities, there are cases where immigrant foreign workers, mostly from Southeast Asian countries, are working as elderly-care workers and nurses. Over the past decade, I have conducted research and published many papers about the challenges for such immigrant workers in these fields, who came to Japan, following the conclusion of the Movement of Natural Persons under an Economic Partnership Agreement (EPA), agreed by the Japanese government with the governments of Indonesia, Philippines and Vietnam. I have also conducted research into the issues receiving institutions face in receiving these workers (See special issue Southeast Asian Studies, 2012, Vol.49:4). As such, what is on the minds of these immigrant care workers and nurses, and what kinds of everyday life do they lead nowadays? During the crisis, how have they perceived the frontline of Japan’s nursing care and medical services, which was often described as “on the verge of collapse” by Japanese mass media.
During late April to mid-May, when a state of emergency was declared all over Japan, I conducted interviews online and by e-mail with an Indonesian nurse, a Filipino care worker, a Vietnamese personnel-service company worker and others, and asked about their circumstances. Based on the above interviews, this article describes their daily lives and how they feel about their work while being concerned about the on-going situation in their home countries during the global crisis.
Everyday Life Working in a Hospital with Infected Patients and Staff: A Day in the Life of an Indonesian Nurse
Since 2008 until now, under the framework of the EPA, a total number of 1,421 nurse candidates from the three countries mentioned above have entered Japan. Among them, 459 candidates have already passed the Japanese National Nursing Examination (Ministry of Health, Labor and Welfare 2020a) and many of them are still working at various hospitals across Japan. One of them, a male Indonesian nurse, Mr. A (in his 30s) works at one in the Kanto region, but he has recently come under a lot of stress. At his hospital, a few of the patients and medical staff became infected with COVID-19. Healthcare workers operating on the floors accommodating infected patients have had to continuously wear medical protective suits. At present, Mr. A is working in a different ward and in addition to wearing masks and washing his hands frequently, he has been wearing disposable gloves more often than before.
Even with a slight fever, nurses have been requested to take two weeks off for observation, in line with regulations. Such cases have also emerged at his workplace. As he is covering a room that was under the supervision of a coworker who came down with a fever, his workload has increased. He stated that “I’m anxious…I don’t know when I could get it or give it to someone.” His words carry a deep sense of reality.
At home, his Indonesian wife and children in elementary and middle school, carry on their “stay at home life.” In order to avoid infecting his family, he sterilizes his clothes and bags completely as soon as he arrives home and takes a bath before coming into contact with them. All members of his family are Muslims, but the nearby mosque is completely closed, so they pray at home. They buy halal food from online shops.
Mr A’s life appears to have been very exhausting both mentally and physically. When I asked him, “do you want to go back to your home country?” he immediately responded “I have never thought about such a thing.” He is a member of the Muslim Association for Indonesian Nurses and Certified Care Workers (インドネシア人看護師・介護福祉士ムスリム協会/IPMI Jepang), which mostly consists of Indonesian settlers in Japan, and he has his good information network among them. He shared that “there is no such move by any other members to return home. Nurses and care workers here have high ethical standards.” He also added that “nurses are given such an education. We cannot just run away.”
The present status of Indonesia also needs to be taken into consideration. At the time of this interview (11 May), the infected population in Indonesia stood at around 14,000 and approximately 960 deaths had been reported. Mr A. said that “I’m not saying Indonesia is safer. But I suppose the lack of nurses could be worse in Japan at the moment. In Indonesia, national regulations are not so strict and many nursing school students are working part-time at hospitals.”
Medical professionals, such as nurses are very crucial in Japan at this present time of emergency. The impact of losing even a single nurse regardless nationality could be quite significant. Since Mr. A and other Indonesian residents in Japan are also distressed by the severe healthcare situation in Indonesia, IPMI Jepang is continuing their activities to distribute medical supplies, including protective suits and masks by tapping into donations they had collected.
Mr. A has rediscovered something about the Japanese medical system through this coronavirus crisis. “It was rather unexpected; we ran out of protective suits. So, we had to improvise with plastic substitutes…. There was group transmission outbreak at a nearby hospital. The situation was not quite good as I had expected.” While he was in Indonesia, he believed, like other Indonesian EPA applicants, that the Japanese medical system was among the best in the world. Thus, in many ways, Japan’s insufficient preparations toward a large-scale infectious disease surprised him even more. Yet, he gave a positive evaluation on the relatively small number of PCR tests carried out in Japan. In his opinion “Japan’s current approach is right. If they test a lot of people at one time and increase patients, it will cripple the capacity to provide appropriate medical services.”

Indonesian certified care worker candidates studying for passing the national examination. They graduated from the nursing school in Indonesia (Photo taken at a social welfare corporation in Tokushima City by the author in March 2018. This photo is not directly related to this report)
Observation by a Filipino Care Worker in Charge of Foreign Staff at an Elderly Care Facility
Group infection outbreaks followed one after another at senior care facilities across Japan. In Fukuoka, the largest city in Kyushu, cluster infections also occurred in several facilities, such as special elderly nursing homes and group homes. In Fukuoka prefecture, industry is centered around Fukuoka city, and has recently faced a labor shortage. As such, they have accepted a considerable number of foreign nationals with designated activities by visa status (those who have entered Japan under EPA) or as technical intern trainings in the field of nursing care. The population of foreign residents in the same prefecture (as of December 2019) is approximately 83,500, an increase of almost 6,400 over the previous year (Ministry of Justice, 2020). This includes a large number of care workers from Southeast Asian nations, such as Vietnam, Myanmar, Indonesia, and Cambodia.
Filipino care workers are also increasing. Some of them have the national license for certified care workers. Ms.Lynette Morales Motoishi (35 years old) is one such qualified worker. She came to Japan in 2010 as an EPA certified care worker candidate. Four years later, she passed the national examination and has now been given the title, “head of foreign staff” working at La Paz (ラ・パス), a long-term care health facility and an affiliate of Jusenkai (寿泉会), a social welfare corporation (Asakura City, Fukuoka). One third (approximately 10) of all the care staff members of this facility are Filipinos.

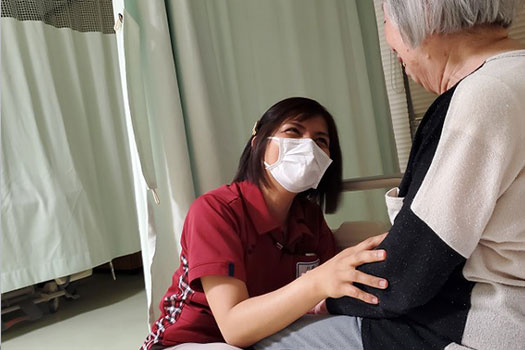
Ms. Lynette Morales Motoishi wearing a facemask regularly in her workplace where she works as a certified care worker and a manager for foreign workers (Photo taken at the long-term care health facility named La Paz in Asakura City by her coworker on 23 May 2020)
La Paz is in a building that accommodates a visiting care home and several other facilities, so they have devised a way to avoid overlaps in the flows of nurses and care workers in charge of the residents and those of other staff members handling other matters. Since the declaration of a state of emergency, they do not allow residents to meet family members, except through online meetings by a computer at their doorway. How does this workplace currently appear to Ms. Motoishi?
“We are washing hands frequently and wearing masks all the time. We take breaks in our own cars (as a measure against group infection). But we feel that it is more or less the same as with a case of normal influenza. Japanese people are feeling more anxious and tenser. Japanese staff are also concerned, saying that the coronavirus would not easily be over, but I would say, it’ll be fine, because the end comes to any infectious disease.”
In Filipino, there is a term, “Bahala na” (everything will work out). Filipino staff in general, seem to possess a more optimistic perspective for the future than their Japanese counterparts. In order to avoid the risk of transmission, she said that Japanese staff are trying to secure some distance from the residents and, as much as possible, shy away from physical contact. On this point, she said, “I have also been careful to avoid physical contact (sukin tacchi) as much as possible, but I just find myself doing it. The residents are used to be touched that way and they might feel uneasy or lonely if we stop touching them”.
She is working as she usually does, trying to soothe the anxieties of the residents by listening to them talk and by taking them out to a balcony. She has realized that the burden of her work is now heavier than before. Still, she said that “staying in Japan is safer.” On the day of this interview (26 April), the number of deaths from the viral infection in her home country had exceeded 500 (351 in Japan at time of the interview), while the situation was evolving into many arrests of lockdown violators who had ignored the strict regulations imposed by the Philippine government.
The EPA workforce, serving as care workers or nurses (including candidates) are generally highly evaluated for their good attitudes toward the residents and patients, including their practice of natural physical contact and strong deference to the elders. It has also been confirmed by the survey we conducted on accepting facilities and hospitals across Japan (e.g. Ogawa et al., 2010). In this sense, the following words of Ms. Motoishi should sound encouraging, not only for the employers but also for the residents: “No Filipino here wants to quit because of the coronavirus situation. Filipinos, wishing to work in Japan would not be decreased in the future.”

A Vietnamese care worker taking care of a Japanese elder person residing at the elderly-care facility (Photo taken in Tokushima Prefecture by the author in March 2018. This photo is not directly related to this report)
Trends in the Rapid Increase of “Care Intern Trainees”
The number of foreign care workers like Ms. Motoishi who came to Japan under the EPA totaled 5,063 by the Fiscal Year 2019 (Ministry of Health, Labor and Welfare, 2020b). Among them, 1,322 people obtained licenses as certified care workers by the end of the same fiscal year (Ministry of Health, Labor and Welfare, 2020c). There is an increasing tendency among those people to invite family members from home countries and to live in Japan, either as long-term or as permanent resident (Ohno 2019).
Notwithstanding, their numbers are still limited and their contribution to solving the lack of care workers in Japan, said to stand at more than 200,000, is still very restricted. As a measure to combat the lack of care workers, the Japanese government established a new visa status called “Nursing Care” (2016) among items of an agenda and added “Nursing Care” to the list of industries under the technical internship program (in 2017). Moreover, in 2019, the government provided a new residential status called “Specified Skilled Worker,” which is defined as involving higher skills than technical intern training. In regards to the specified skilled workers for the nursing care sector, the government is planning to accept up to 60,000 foreign personnel over a five-year period between 2019-23 from neighboring Asian countries.
Among them, specified skilled workers in the nursing care sector are not only required to pass the Japanese language test, but also nursing care related exams as a criterion for recruitment, yet the possibility of switching workplaces after coming to Japan are generally unpopular among employers. As a result of this, acceptance of workers is not proceeding on the scale originally planned by the government. On the other hand, technical intern trainees in the care sector, who are basically not allowed to change his/her workplace, tend to be rapidly increasing over the last few years. According to a survey on approximately 9,000 care businesses across Japan, conducted in 2018 by “Care Work Foundation [介護労働安定センター]”, a public interest incorporated foundation, the number of employers, who had already accepted foreign workers were only 233, while those that responded that they are “considering to utilize their workforce for the future” amounted to 1,204. Two thirds of them, or 785 businesses, turned out to be planning to accept them as technical intern trainees (Care Work Foundation, 2019).
Among “care technical intern trainees” to Japan, those from Vietnam are particularly increasing. For instance, a major recruiting agency in Vietnam, “Hoang Long Investment Construction and Manpower Supply Joint Company” (based in Hanoi) has already dispatched 718 (91.4% of them were female) technical intern trainees engaging in care work to Japan. Elderly-care is work that requires a certain level of communication ability, so the company provides a year of on-site training, which is longer than other fields, and only those who pass level 4 Japanese Language Proficiency Test (JLPT) are allowed to go to Japan. Regardless, there are a large number of applicants for technical intern training in the nursing care sector, and one of the factors is a steady income. According to Mr. Pham Ngoc Binh, the director of the Japan business division of the same company, the actual income of the basic salary for care services is around 135,000 yen, but many night shifts and overtime would provide them with extra monthly earnings, and on top of that, they can receive a bonus, which is rare for technical interns in other fields, thus it tends to encourage motivations to apply. There are also many young Vietnamese who have applied to the same training program because they recognize that in Vietnam, the necessity of elderly-care businesses will be higher in the future as the country is one of the most rapidly aging societies in the world (Mr. Pham in response to my questions sent by e-mail, 14 and 15 May, 2020).
The same company had originally planned to send more technical interns to Japan in 2020 over the previous year: about 1,000 trainees only for the nursing care sector. This was equivalent to a third of the total number of technical intern trainees they were dispatching.

Vietnamese technical intern trainees receiving on-the-job training before their going to Japan (Photo taken at the training center of Hoang Long Investment Construction and Manpower Supply Joint Company in Hanoi around Nov. 2019. This photo was provided by the company)
The coronavirus crisis did not spare Vietnam, however, they were among the first in the world to take quarantine measures from early February against those entering the country from nations with a large number of infected cases, such as China, and subsequently placed strict regulations on immigration for both locals and foreigners. Though the training facilities of Hoang Long were also temporarily closed, the number of deaths from infection remained zero even in late May, proving that Vietnam has been successful in containing the spread of the infection. Therefore, the company had shifted to online lessons, but it was back to normal operations by the beginning of May.
In Japan, on the contrary, infections have continued to spread, mostly in urban areas, with the death toll exceeding 700 at the time of exchanging e-mails with Mr. Pham. Some of the trainees sent from Hoang Long living in Japan were so afraid of infection that they wanted to return to their home country as early as possible before the expiration day of their contracts. Later, however, since there was a sudden fall in the number of new coronavirus cases in Japan after the middle of April, many of them had second thoughts about going home. Luckily, there have been no case of transmission at any of the care facilities across Japan where those trainees from the same company were assigned to, and they are reportedly continuing steadily with their intern programs (Reply from Mr. Pham, 13 May, 2020).
The Wider Acceptance of Foreigners to Care Industry: An Unchanging Trend?
Between 2008 to 2009, when the Lehmann Shock tore across the world, Japan was observing a wave of what was called, “Yatoi-dome” and “Haken-giri”: the former refers to the denial of contract renewals for non-regular employees and the latter to the layoff of temporary workers. As a result, many foreign workers on unstable employment conditions lost their jobs. Brazilians (the vast majority were Japanese descents), who lived in Japan, mostly working in the manufacturing industry, later saw their population diminish by more than 100,000. Similarly, during this coronavirus crisis, it has been reported that foreign workers in manufacturing and other sectors had their employment terminated through “Yatoi-dome” and “Haken-giri” as mentioned above. Such a situation, however, does not apply to foreign workers, as far as they are in medical or nursing care sectors, whose population has continued to increase in Japan since the Lehman Shock. On the contrary, their importance as “essential workers” under emergency situations has been reaffirmed in each local community and therefore, local governments and employers are trying hard to retain them at their workplaces, even by providing special allowances like they do to other Japanese staff.
In the U.S. and countries in Europe, where the death toll has exceeded tens-of-thousands, the collapse of medical and nursing care services occurred in various places, and a considerable number of deaths have been reported not only for the patients and residents, but also for workers in those fields. In Japan, the deaths of residents and patients at care facilities and hospitals also followed. Yet with care workers and nurses, and those among them who became infected, no cases of death have been reported at the time of writing (22 May, 2020). As far as my recent interviews with one responsible person at the Japan International Corporation of Welfare Services (JICWELS), in charge of the EPA project and recruitment agencies for technical intern trainees based in Vietnam and Myanmar have shown, there is no conspicuous move among EPA candidates and care intern trainees in Southeast Asian countries, standing by in their home countries to be employed in Japan, to cancel their plans to come to Japan.
Once the spread of viral infection subsides in Japan and other Asian countries and as borders reopen, I can assume that the movement toward the wider acceptance of care workers from neighboring Asian countries, especially elderly-care workers coming to Japan will be back on track.
4 June, 2020
(Translated by Yoshida Chiharu)
References
- Care Work Foundation [介護労働安定センター]. 2019. Results of Research on the Actual Conditions of Care Work for Fiscal Year 2018 [平成30年度『介護労働実態調査』の結果] http://www.kaigo-center.or.jp/report/pdf/2019_chousa_kekka.pdf (Accessed 20 April, 2020).
- Mainichi Shimbun (Morning ed.). 13 May, 2020. Editorial, Corona and Elderly-Care [社説 コロナと高齢者ケア].
- Ministry of Health, Labour and Social Welfare (MHLSW). 2020a. Results of National Examinations for Registered Nurses under Economic Partnership Agreement (EPA) for Last 12 Years [経済連携協定(EPA)に基づく外国人看護師候補者の看護師国家試験の結果(過去12年間)] https://www.mhlw.go.jp/content/10805000/000610408.pdf (Accessed 30 April, 2020).
- ーーー. 2020b. Transition of Numbers of Accepting Persons [受入れ人数の推移], https://www.mhlw.go.jp/content/000595174.pdf, (Accessed 30 April, 2020).
- ーーー. 2020c. Results of the 32nd National Examination for Certified Care Workers. [第32回介護福祉士国家試験結果] https://bit.ly/2WGvtvU (Accessed 30 April, 2020).
- Ministry of Justice (MOJ). 2020. Concerning the Numbers of Foreign Residents in Japan as of the End of2019” [令和元年末現在における在留外国人数について]. http://www.moj.go.jp/nyuukokukanri/kouhou/nyuukokukanri04_00003.html (Accessed 20 April, 2020).
- NHK NEWS WEB. 8 May 2020. The Crisis of Care Collapse due to COVID-19: What happened at Care Facilities? [新型コロナで“介護崩壊”の危機?高齢者施設でいま何が] https://www3.nhk.or.jp/news/html/20200508/k10012422701000.html (Accessed 15 May, 2020).
- Ogawa, Reiko et al. 2010. A Follow-up Survey on Hospitals and Long-Term Care Facilities Accepting The First Batch of Indonesian Nurses/Certified Care Worker Candidates (1): Analysis on the Current Status and Challenges [来日第1陣のインドネシア人看護師・介護福祉士候補者を受け入れた全国の病院・介護施設に対する追跡調査(第1報)―受け入れの現状と課題を中心に]. Bulletin of Kyushu University Asia Center [九州大学アジア総合政策センター紀要], Vol.5:85-98.
- Ohno, Shun, 2019, “Long-Term Care Migrants Becoming Long-Term Residents in Japan: Their Problems and Consciousness 10 Years after the Economic Partnership Agreement(EPA) Entered into Force”[日本定住化が進む『介護移民』―経済連携協定(EPA)での受入れ開始から10年目の現状と課題」、The Annual Review of Migration Studies[移民研究年報], Vol. 25:113-125.
Shun Ohno is professor of the Department of Global Citizenship Studies, Seisen University, and affiliated professor at Center for Southeast Asian Studies, Kyoto University (Department of Global Humanosphere). He was the editor for a special issue in the journal of Southeast Asian Studies (2012, Vol.49:4) published by CSEAS, dealing with the “International Migration of Southeast Asian Nurses and Care Workers to Japan under Economic Partnership Agreements.”
Citation
Shun Ohno. 2020. “Southeast Asian Workers on the Ground of Pandemic-Stricken Medical and Nursing Care Services in Japan: Their Daily Lives and Concerns” CSEAS NEWSLETTER, 78: TBC.